Custom ski orthotics – Are you ready for a ski season?
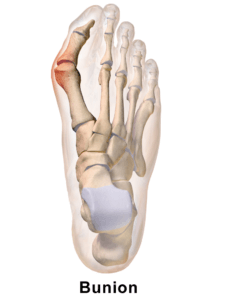
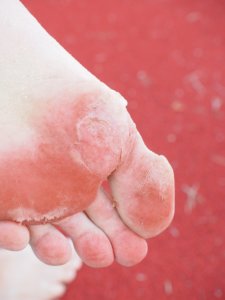
Arch pain is a fairly common problem for skiers. While it is seen more frequently in a flat foot type it can happen in any foot type. The feet work very hard inside your ski or snowboarding boots particularly when skiing moguls, frequent turns or in icy conditions; as is often seen in the North East.